Research Article - (2021) Volume 12, Issue 3
Background: Medical Nutrition Therapy (MNT) plays a very important role in diabetes management if advised to the patient with proper counselling.
Objective: The objective of this prospective study was to determine efficacy and safety of MNT in improving glycemic control in pre-diabetic and diabetic population as monotherapy and as added therapy with ongoing anti-diabetic drugs.
Methods: Adult participants with Type 2 Diabetes Mellitus (T2DM) and pre-diabetics (HbA1c>6.0) were selected for the study. The MNT as Oral Nutrition Supplement was supplemented to their diet with and without concomitant medications. The primary endpoint was change in HbA1c, fasting and postprandial blood glucose. Secondary endpoints were change in lipid parameters such as cholesterol, high density lipids (HDL), low density lipids (LDL) and triglycerides. Mean change in the parameters were analysed using paired t-test with significance value of 5%. This was a 24-week, multi-centre, prospective, observational study.
Results: A total of 313 patients completed the study until 24 weeks and a statistically significant reduction in HbA1c levels was seen from baseline to 12 weeks (8.6% to 7.7%; p<0.001) and at 24 weeks (8.6% to 7.1%: p<0.001), respectively, due to only MNT intake. Similar significant reduction in fasting glucose (167.4 to 119.4 mg/dL) and post-prandial glucose parameters (232.1 to 156.2 mg/dL) were also observed at both 12 and 24 weeks, respectively due to only MNT intake. The data showed that MNT is effective as both stand alone and as add-on food supplement to ongoing therapies and safe to consume.
Conclusion: There was significant reduction in levels of hyperglycemic and lipid parameters in pre-diabetics and diabetics upon taking monotherapy or as an added therapy along with anti-diabetic drugs.
Medical nutrition therapy; Diabetes; India; Type 2 diabetes mellitus
Abbreviations: MNT: Medical Nutrition Therapy; T2DM: Type 2 Diabetes Mellitus; HDL: High density lipids; LDL: Low density lipids; IDF: International Diabetes Federation; BMI: Body Mass index; AEs: Adverse events; FBG: Fasting glucose; PPG: Post-prandial glucose
Over the world, diabetes has a major impact on individuals and their families as it is a serious and chronic disease. It stands in top 10 causes for death in adults.The International Diabetes Federation (IDF) has estimated to have 578 million people living with diabetes by 2030 [1].
The complications related to diabetes leads to most of the morbidity and mortality. The most important risk factor in uncontrolled diabetes is the microvascular and macrovascular complications [2]. The microvascular complications affect the eye especially the inner part of eye leading to diabetic retinopathy. Involvement of the kidney and peripheral nerves, leads to diabetic nephropathy and diabetic neuropathy, respectively. The macrovascular complications affect the brain, heart and peripheral arteries, leading to cardiovascular disease and peripheral vascular diseases [3].
The major drivers for rapidly changing dynamics of T2DM include unhealthy modern diet and low activity patterns. Another reason for rising trend in diabetes include replacement of traditional Indian meals such as legumes, coarse cereals, whole grains, fruits and vegetables with foods having refined carbohydrates, added sugars and high intake of fats [4].
Additionally, expansion of fast food chains and supermarkets has made it very easy to access westernized foods [4]. Studies suggest that due to improper education and guidance, diabetics completely remove dietary carbohydrates and include bitter foods which potentially lower blood glucose levels [5,6]. Due to these misbeliefs, the dietary guidance is ignored and it stands as a barrier to pharmacologic treatment attempts as well.
For the prevention and management of diabetes mellitus, an appropriate lifestyle and dietary changes are required. An essential component of diabetes management includes Medical nutrition therapy (MNT) along with counselling the patient. MNT comprises of nutritional assessment, advice and follow-up, for prevention and/or management of disease, by a qualified or trained health care provider. It includes dietary, nutritional and culinary advice. It comprises of both home-made food and medical-grade formulations.In the context of T2DM, MNT aims to manage both dysglycemia and adiposity, through nutritional intervention [7].
Evidences suggest that diabetic patients receiving MNT show decline in blood glucose parameters such as HbA1c. Such interventions provide improvement in overall health outcomes, reductions in cost of therapy and increase in quality of life [8-13]. Thus, our aim was to analyse safety and efficacy of MNT in glycemic management of diabetics and pre-diabetics.
A prospective observational study was carried out where total of 325 adult participants were included, of which, 191 were males and 134 were females. Inclusion criteria include participants with HbA1c levels>6.0, having no other co-morbidities or medications, except anti-diabetic drugs. Participants undergoing any other trials or surgery were excluded from the study.
The study was performed in compliance with the principles of the Declaration of Helsinki, in accordance with the International Conference of Harmonization Guideline for Good Clinical Practice, and in accordance with applicable regulatory requirements. All participants provided a written informed consent.
Endpoints
Body Mass index (BMI) for each participants was calculated. The primary endpoint was mean change in HbA1c levels, FBG and PPG from baseline to week 12 & 24 where MNT (VidavanceTM) was supplemented as monotherapy or add-on therapy with ongoing oral antidiabetic agents. Secondary endpoints were change in lipid profile parameters (cholesterol, LDL, HDL and triglycerides) from baseline to week 12 & 24. Adverse events (AEs) were monitored during the study period.
Statistical analysis
Descriptive statistics for continuous variable and frequency with percentage for categorical variables were performed. Data were analysed and the mean data along with the standard deviation (SD) were subjected to statistical analysis using paired t-test with significance value of 5%.
Total 325 participants enrolled in the study out of which 313 participants (96.3%) completed the study until the end of 24 weeks. Figure 1 presents the patient disposition. Compliance rate was high among participants, with minimal drop out.'
Demographics
The mean age and BMI of the study participants were 53.5 ± 11.1 years and 28.65 ± 1.45 kg/m2, respectively. The participants were divided into two groups. Group I (n=157) comprised of patients taking MNT alone and Group II was taking concomitant anti-diabetic therapies like Metformin, Voglibose, Glimepiride, Sitagliptin, sulphonyl urea along with MNT(n=156) where ‘n’ stands for number of patients.
Out of 157 participants from Group I, 141 were diabetic and 16 were pre-diabetic and out of 156 participants from Group II, 149 were diabetic and 7 were pre-diabetic (Figure 1).
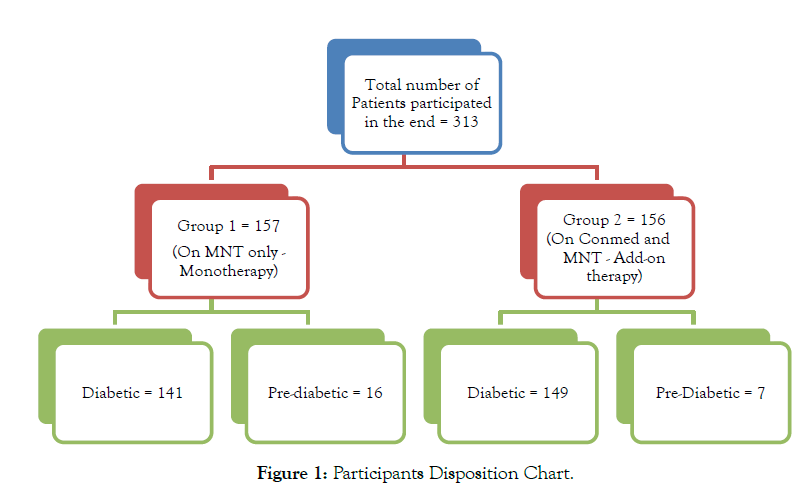
Figure 1: Participants Disposition Chart.
Study participants were either taking concomitantly (Conmed) anti-diabetic therapies with MNT (n=156), or MNT alone (n=157). Glucose metabolism parameters & lipid profile was assessed at baseline, 12 and 24 weeks. Subcategorized into pre-diabetic (HbA1c<6-6.5) and Diabetic (HbA1c>6.5).
Efficacy
The mean values of glycemic parameters (HbA1c, FBG, and PPG) for Group I (Monotherapy) and Group II (concomitant therapy) are shown in Table 1. Mean HbA1c was 8.81% (SD=0.37) at baseline which reduced to 7.80% (SD=0.96) at week 12 and 7.16% (SD=0.84) at week 24 with noted in Group I. In Group II, it was 8.39 (SD=1.17) at baseline, 7.69 (SD=0.80) at week 12 and 7.13 (SD=0.79) at week 24. The differences in the mean HbA1c in both the groups were found to be statistically significant (p<0.001) (Table 1).
Statistically significant reductions in mean FBG values and PPG values were seen in both the groups as shown in Table 1. Similar significant changes (p<0.001) were seen in these three parameters for pre-diabetics group as well (Table 2). All the above parameters are graphically presented in Figure 2.
| Glucose Metabolism Parameters | Baseline | 12 Weeks | 24 Weeks | |||
|---|---|---|---|---|---|---|
| HbA1c (%) | Group I | 6.15 ± 0.16 | 6.09 ± 0.26 | 5.94 ± 0.23 | ||
| Group II | 6.2 ± 0.12 | 5.85 ± 0.54 | 5.7 ± 0.55 | |||
| FBG (mg/dL) | Group I | 115.75 ± 14.19 | 102.08 ± 8.86 | 110.75 +25.5 | ||
| Group II | 117.14 ± 18.72 | 105.28 ±20.99 | 98.42 ± 24.79 | |||
| PPG (mg/dL) | Group I | 147.83 ± 25.7 | 135.16 ± 13.48 | 128.25 ± 17.78 | ||
| Group II | 144.71 ± 18.41 | 131.14 ± 26.14 | 120 ± 22.03 | |||
Table1: Table showing mean HbA1c, FBG and PPG values in Group I and Group II in diabetics (HbA1C>6.5).
| Glucose Metabolism Parameters | Baseline | 12 Weeks | 24 Weeks | |||
|---|---|---|---|---|---|---|
| HbA1c (%) | Group I | 6.15 ± 0.16 | 6.09 ± 0.26 | 5.94 ± 0.23 | ||
| Group II | 6.2 ± 0.12 | 5.85 ± 0.54 | 5.7 ± 0.55 | |||
| FBG (mg/dL) | Group I | 115.75 ± 14.19 | 102.08 ± 8.86 | 110.75 +25.5 | ||
| Group II | 117.14 ± 18.72 | 105.28 ±20.99 | 98.42 ± 24.79 | |||
| PPG (mg/dL) | Group I | 147.83 ± 25.7 | 135.16 ± 13.48 | 128.25 ± 17.78 | ||
| Group II | 144.71 ± 18.41 | 131.14 ± 26.14 | 120 ± 22.03 | |||
Table 2: Table showing mean HbA1c, FBG and PPG values in Group I and Group II in Pre-diabetics (HbA1C 6-6.5).
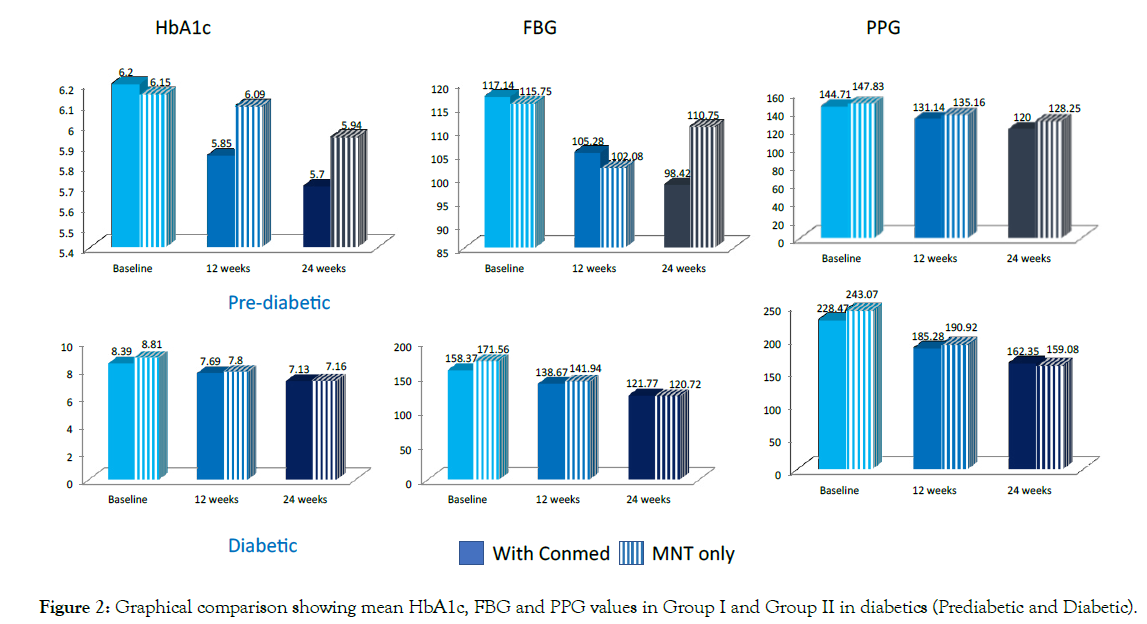
Figure 2: Graphical comparison showing mean HbA1c, FBG and PPG values in Group I and Group II in diabetics (Prediabetic and Diabetic).
Statistically significant reduction in HbA1c levels is seen from baseline to 12 weeks (8.81 to 7.8; p<0.001) and at 24 weeks (to 7.16: p<0.001) in both groups I and II in diabetics.
Similar significant changes (p<0.001) was seen in the three parameters in both groups for pre-diabetics as well.
The values obtained were comparable with statistically significant reduction in HbA1c levels, fasting glucose and post-prandial glucose from baseline to 12 weeks and at 24 weeks.
The effect of MNT consumption also noted on lipid parameters which included levels of cholesterol, HDL, LDL and triglycerides. Mean cholesterol levels was 195.02% (SD=43.46) at baseline which decreased to 182.9% (SD=28.22) at week 12 and 154.13% (SD=30) at week 24 as noted in Group I and in Group II, it was 195.6 (SD=34.59) at baseline, 177.3 (SD=32.57) at week 12 and 158.59 (SD=23.52) at week 24. The differences in the mean cholesterol in both the groups were found to be statistically significant (p<0.001) (Table 3).
| Lipid Profile Parameters | Baseline | 12 Weeks | 24 Weeks | ||
|---|---|---|---|---|---|
| Cholesterol | Group I | 195.02 ± 43.46 | 182.9 ± 28.22 | 154.13 ± 30 | |
| Group II | 195.6 ± 34.59 | 177.3 ± 32.57 | 158.59 ± 23.52 | ||
| LDL | Group I | 133.94 ± 34.06 | 123.41 ± 24.2 | 113.92 ± 37.54 | |
| Group II | 125.53 ± 24.9 | 114.44 ± 24.26 | 104.35 ± 27.35 | ||
| HDL | Group I | 76.71± 133.43 | 49.94 ± 32.23 | 47.13 ± 22.89 | |
| Group II | 36.75 ± 11.56 | 36.74 ± 9.19 | 37.14 ± 7.24 | ||
| Triglycerides | Group I | 185.26 ± 64.47 | 170.26 ± 43.45 | 129.06 ± 30.07 | |
| Group II | 185.61 ± 63.23 | 157.55± 36.47 | 139.64 ± 31.98 |
Table 3: Table showing mean Cholesterol, LDL, HDL and Triglycerides values in Group I and Group II in diabetics (HbA1C>6.5).
Similar significant change (p<0.001) was seen in these parameters for pre-diabetics as well (Table 4).
| Lipid Profile Parameters | Baseline | 12 Weeks | 24 Weeks | ||
|---|---|---|---|---|---|
| Cholesterol | Group I | 197.83 + 61.78 | 185 + 15.5 | 144.8 + 50.8 | |
| Group II | 200.67 + 31.77 | 166.66 + 32.53 | 137.66 + 11.67 | ||
| LDL | Group I | 116.35 + 44.49 | 131 + 52.89 | 102 + 38.45 | |
| Group II | 148.5 + 55.48 | 142 + 36.36 | 85 + 45.82 | ||
| HDL | Group I | 39.5 + 9.84 | 32.5 + 0.7 | 36.25 + 9.17 | |
| Group II | 29.33 + 8.32 | 35 + 8.88 | 36.33 + 10.01 | ||
| Triglycerides | Group I |
127.4 + 24.18 | 127 + 7.07 | 111.4 + 36.95 | |
| Group II | 125 + 120.2 | 175 | 100 |
Table 4: Table showing mean Cholesterol, LDL, HDL and Triglycerides values in Group I and Group II in pre-diabetics (HbA1C>6-6.5).
Numerical reduction in levels of lipid profile parameters is also seen in both the diabetic groups
Similar statistical significant reduction in glycemic parameters were also observed in the concomitant groups.
The data showed that MNT (ONS) is effective as both monotherapy and as concomitant or add-on therapy to reduce the glycemic parameters from baseline to end of the study (24 weeks) was seen.
Safety
No adverse events were observed till 24 weeks of follow-up in any of the participants, showing it was safe for consumption.
MNT includes description of procedures for providing nutritional recommendations to an individual by a healthcare professional which considers the patient’s personal, cultural and lifestyle preferences so that required target can be achieved towards the treatment goals. Essential components of MNT include assessment, nutrition diagnosis, education and counselling, and monitoring with ongoing follow-up which is required to support long-term lifestyle changes, evaluate outcomes and modification of interventions as and when required.
The optimal treatment to obtain fair glycemic control is the goal of antidiabetic therapies. However, along with the antidiabetic drugs, modifications in lifestyle and dietary precautions are also important, where MNT plays an important role. In this observational study, there were significant reductions in HbA1c, FBG and PPG at the end of the 24 weeks of study. A 1.0% & 1.64% reduction in HbA1c due to consumption of MNT at 12 and 24 weeks, respectively in diabetics. Similar reduction was also seen in group of participants undergoing concomitant medications. A study conducted by Nisak et al stated that there was reduction in HbA1c levels by 0.4% (7.6 ± 1.2 to 7.2 ± 1.1%, p<0.001) at 12 weeks after use of MNT in diabetic patients. They also noted that baseline HbA1c levels before the intervention affected the extent of change MNT could have on glycemic control in T2DM [14]. Johnson and Valera reported six-month retrospective chart audit of T2DM patients whose blood glucose levels decreased 33.5% after receiving nutrition therapy. Also, the mean total weight reduction in patients was about 2.05 kg [15].
Johnson and Thomas reported decrease in levels of HbA1c by 20% in the patients who received MNT intervention over a period of 12 months [16]. Christensen et al. carried out a retrospective chart review where they found significant difference (mean pre-education HbA1c 9.35% ± 2.12 to mean post-education HbA1c 7.70% ± 1.53, P<0.000) in contribution of medical nutrition therapy and diabetes self-management education to diabetes control in the time span of 3 months [13]. This study results were in accordance with other studies and thus, support the evidence that MNT plays a very important role in diabetes management. Overall MNT intake was found to be efficacious in reducing blood hyperglycemic parameters along with lipid profile parameters.
Among all glycemic parameters, PPG plays an important role in lowering the levels of HbA1c. Hence, decrease in PPG will lead to greater reductions in HbA1c along with decrease in FBG. So, it is very important to control the levels of PPG [17]. Various studies have reported strong association of PPG with diabetes complications and other changes such as cardiovascular and cerebrovascular complications, oxidative stress, carotid intimal thickness and endothelial dysfunction [18,19]. This study showed a significant reduction in PPG and FBG levels, providing a better overall glycemic control.
The macro and micro vascular complications are the side-effects of un-controlled glycemic levels. Diabetes induced dyslipidemia includes hypercholesterolemia; hypertriglyceridemia and elevated LDL cholesterol are few microvascular complications started to rise when diabetes gets uncontrolled. High prevalence of dysplipidemia plays a major role in developing cardiovascular and cerebrovascular diseases in diabetics. Hence, it’s crucial to monitor and maintain the lipid parameters during anti-diabetic therapies. Our data showed that consumption of MNT not only significantly reduces the glycemic parameters, but also reduced the increased lipid profile parameters like LDL, Cholesterol and Triglycerides at the end of 24 weeks of study. This extends the use of MNT in controlling the diabetes associated cardiac complications as well.
The goal of MNT is to also promote and support healthy eating patterns. It emphasizes on variety of numerous nutrient-dense foods in the portion sizes which are appropriate to improve overall health. The aim differs from individual to individual which is based on age, duration of diabetes, health history and current health conditions. The focus is to improve HbA1c levels, blood pressure, and cholesterol levels. Other associated goals include maintenance of body weight, prevention of diabetes complications, looking into individual nutrition needs, behavioural changes and providing diabetics with practical tools so that day-to-day meal planning can be done [17].
MNT if given in pre-diabetics helps to reduce the transformation of pre-diabetes to diabetes. For pre-diabetics, it is a cost-effective measure as it helps in improving outcomes as well as it also improves quality of life of pre-diabetics. Out data showed that consumption of MNT in pre-diabetics reduced HbA1c, FBG, and PPG levels at 24 weeks of the use. The use of dietary strategies for prevention of diabetes has been successfully implemented by various studies such as the Finnish.
It should be made sure that the MNS intervention therapy is taken from a registered dietitian or nutrition expert. Doctors should encourage their patients to take health plan to achieve treatment benefits early. The MNS intervention therapy is helpful for prediabetic patients as timely MNS intervention therapy can prevent them from getting diabetic [18]. Diabetes Prevention Study, the Diabetes Prevention Program (DPP) and the Nurses’ Health Study. According to DPP study, the incidence of T2DM can be reduced to 58% by modification in life-style structure. Various studies state that with MNT have shown to decrease rate of incidence of diabetes. The benefit of sticking to a balanced diet along with regular physical activity is improved sensitivity to insulin and preservation of beta cells [3].
This study provides a new insight on how MNT can manage the glycemic parameters and improve overall health conditions. We observed that MNT is effective to manage diabetes not only as monotherapy but as add-on therapy as well and were safe to consume.
In the present study, the time duration of 24 weeks of treatment could be increased further for better and long-term monitoring of the MNT effect.
Overall, it can be concluded that MNT provides an important treatment option to pre-diabetic and diabetic patients. MNT should be considered as monotherapy or add-on therapy, in addition to recommendations to increase physical activity and change in life-style for better management of T2DM. VidavanceTM was found to be efficacious in reducing hyperglycemic parameters: HbA1c reduced by 0.9% at 12 weeks and by 1.5% at 24 weeks, due to only MNT. Significant reduction in fasting and post-prandial glucose was also seen.
This work was carried out in collaboration between all authors. Authors KS and BS designed the study. All authors conducted research and analyzed data. Authors MH and MC managed the literature searches and wrote the first draft of the manuscript. All authors read and approved the final manuscript. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work, and have given final approval for the version to be published. Authors thank Mr. Tanmay Agrawal and Dr. Atul Mishra for executing the study. Medical writing and editorial support in the preparation of this article was provided by Dr. Punit Srivastava of Mediception Science Pvt Ltd.
No conflict of interest.
Funding Funding was done by Signutra®, New Delhi.
Citation: Kalra S, Banzal S, Mahapatra H, Mehndiratta C (2021) Medical Nutritional Supplement Improve Glycemic Control in Pre-Diabetics and Type 2 Diabetics: A Prospective Study in Indian Population. J Diabetes Metab 12:868.
Received: 02-Mar-2021 Published: 02-Apr-2021, DOI: 10.35248/2155-6156.21.12.870
Copyright: © 2021 Kalra S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.