Case Report - (2023) Volume 8, Issue 1
Subcutaneous Emphysema is a condition that occurs after air intrusion into soft tissues. While it is easily recognized when seen secondary to surgical procedures, massive air in cases of asymptomatic pneumomediastinum, and pneumothorax may mimic angioedema. Subcutaneous emphysema, which can be confused with angioedema at first glance, can be easily distinguished by physical examination including palpation and detailed history. In the Covid 19 pandemic, physical examination is more neglected due to the infection concerns of the physician and the patient, which can lead to delay in diagnosis, wrong treatment, and fatal results. In our case, the patient who presented to the emergency department was diagnosed with angioedema without physical examination, and the patient was given inappropriate treatment. With this case, we wanted to emphasize that despite the developing technology, physical examination and clinical history are still the basic and low-cost diagnostic methods.
Subcutaneous emphysema • Angioedema • Covid 19 • Pneumothorax • Pneumomediastinum
Subcutaneous emphysema is the result of accidental air intrusion into soft tissues. It is mostly a complication of surgical interventions on the oropharynx, esophagus, and trachea, but may rarely be associated with an underlying pneumothorax or pneumomediastinum [1]. Recently, cases of spontaneous pneumothorax, pneumomediastinum, and subcutaneous emphysema are increasing in the Covid 19 pandemic, even in asymptomatic coronavirus infections. Subcutaneous emphysema can easily be confused with angioedema at first glance, but it can be distinguished from each other by physical examination and clinical history [2-4].
We present a 66-year-old male patient who presented to the emergency department with the complaint of new-onset facial swelling. He was treated with antihistamines, systemic steroids, and intramuscular adrenaline in order, in the emergency department with the diagnosis of angioedema. No detailed history was taken from the patient and no physical examination was performed. Since there was no improvement in the patient's complaints, the patient was consulted with the dermatology department. On physical examination, diffuse facial swelling was found predominantly involving the periorbital region, bilateral cheeks, and neck region with sparing the lips, and ecchymoses on the right backside of the patient. The patient did not have other complaints such as shortness of breath, itching, and rash. There was no history of any food allergy, drug allergy, or similar such episodes in the past, however, before his complaints, he had a history of falling down a ladder a week ago. The ecchymosis on the back occurred as a result of falling, but the patient did not tell because he thought it was unrelated to his complaint. On palpation of the lesions, crepitation was observed in the upper part of the trunk, the dorsum of the left hand, and the face, additionally, an air bubble was present in the lateral cantus of the right eye (Figure 1). Chest X-ray (posteroanterior view) showed widespread pneumomediastinum, diffuse opaque lines/shadows of gas density suggesting emphysema in the subcutaneous region of the neck and trunk, besides minimal right-sided pneumothorax (Figure 2). A thoracostomy tube was inserted into the right lung by the thoracic surgeon and the patient was discharged in full recovery after 5 days.
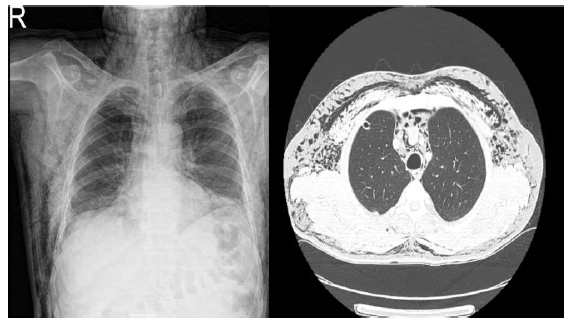
Figure 1: Diffuse facial swelling involving the periorbital region, bilateral cheeks, and neck region with sparing the lips (left), air bubble in the lateral cantus of the right eye (right).
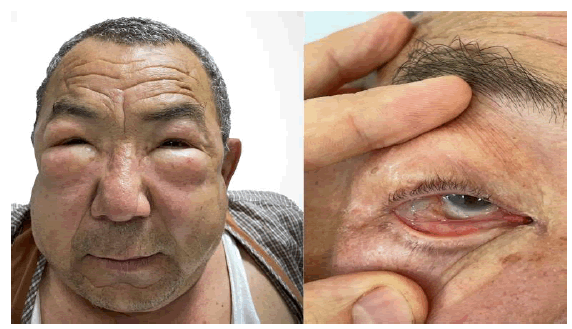
Figure 2: Widespread opaque lines/shadows of gas density suggesting emphysema in the subcutaneous region of the neck and trunk (left), subcutaneous air accumulation in the anterior chest wall and bilateral axilla, and air leak in the superior anterior mediastinum compatible with pneumomediastinum (right).
Subcutaneous emphysema can be easily differentiated from angioedema when seen after surgical operations such as head and neck surgery and dental interventions. Involvement of the eyelids with sparing of the lips on the face is a clue for the diagnosis, air bubbles on the conjunctival examination, detection of crepitation on palpation, and opacities on the xray makes the diagnosis [5]. However, it may not be considered first in the diagnosis when it is seen following pneumomediastinum and pneumothorax that do not impair hemodynamics as in our case. In fact, in our case, as a result of not performing a physical examination in which the whole body of the patient was evaluated by the first physician, and not taking a detailed history, a wrong diagnosis was made and unnecessary treatment was given. In a study conducted with twenty-seven doctors, 63% of the participants stated that the oversight was caused by not performing a physical examination. As a result of insufficient physical examination, delay in diagnosis occurred in seventy-six percent of the patients [6]. In the Covid 19 pandemic, we observe that physical examination is neglected more compar-ed to the past because of infection concerns. In a publication, a set-up in which the patient and the doctor are in different cabins has been proposed to examine the outpatients [7]. Also, in this period, teledermatology applications and reports are becoming more popular, especially in the field of dermatology [8]
Despite all the developing technology, the art of physical examination still maintains its importance as a cheap, basic diagnostic method. Taking a detailed history and performing a physical examination including palpation by following the Covid 19 infection precautions, both prevent the administration of wrong treatments, misdiagnosis and may be life-saving for some patients
[Google Scholar] [Cross Ref]
Citation: Soyugür, A., et al. Importance of Differentiating Subcutaneous Emphysema from Angioedema. Dermatol. Case Rep. 2023, 08(1), 001-002
Received: 06-Feb-2022, Manuscript No. dmcr-23-21714;; Editor assigned: 08-Feb-2022, Pre QC No. dmcr-23-21714 (PQ); Reviewed: 10-Feb-2022, QC No. dmcr-23-21714 (Q); Revised: 12-Feb-2022, Manuscript No. dmcr-23-21714 (R); Published: 15-Feb-2022
Copyright: ©2023 Soyugür, A. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.