Review - (2019) Volume 7, Issue 4
Pulmonary Rehabilitation (PR) is an underutilized service for patients with COPD. This integrative review aims to compile current evidence-based research about the benefits of physician generated PR referrals for the moderate-tosevere COPD patient.
An integrative review of the literature was initiated by searching these electronic databases: PubMed, The Cochrane Library, Cumulative Index to Nursing and Allied Health Literature (CINAHL), Nursing and Allied Health, Health and Management, and Health and Wellness. The articles utilized for this review spanned from the years of 2010- 2018, except for two articles that were published in 2008. Types of articles included in this integrative review include randomized controlled clinical trials, quantitative studies, and qualitative studies. The number of studies included in this integrative review is 33.
Referral to PR programs is recommended by COPD GOLD Guidelines and the American Thoracic Society. Physician PR referral rates is as low as 3%-16% due to health care provider and patient lack of awareness of both the benefits of PR and the PR referral process. Authors of these studies posit that providers who are knowledgeable of the PR referral process are more likely to initiate PR referrals.
Findings from this integrative review are would be beneficial to the creation of a proposal to increase PR referrals in the primary care setting. Health care provider and patient limited knowledge about the benefits of PR for the moderate-to-severe COPD patient poses a clinical practice gap. Continued research centered around benefits of PR, barriers to referral, and a streamlined PR referral process is imperative to improve PR uptake and utilization.
Pulmonary rehabilitation; Chronic Obstructive Pulmonary Disease (COPD); Adult; Global Initiative for Obstructive Lung Disease (GOLD) guidelines; Outcomes; Referral process; Hospitalization; Adherence and the MeSH term pulmonary disease chronic obstructive
Chronic Obstructive Pulmonary Disease (COPD) is a progressive condition of limited airflow affecting the respiratory system, making breathing more difficult due to increased airway inflammation and decreased oxygen/carbon dioxide exchange [1]. COPD is predicted to be the third leading cause of death worldwide by the year 2020 [2]. COPD is an irreversible and progressive disease, which often leads to depression and poor life satisfaction [3]. COPD affects approximately 12 million people in the United States annually, but there are as many as 12 million more people who have yet to be diagnosed [4]. Approximately five million people worldwide, predominantly 65 years of age and older, will die annually from complications of COPD and from progressive limitations in physical activity, social interactions, and independence [5]. Presenting symptoms that most commonly affect people diagnosed with COPD include increased production of sputum, shortness of breath, and cough [6].
Smoking is the predominant risk factor in the COPD population, but inhalation of biomass fuels, childhood exposure to cigarette smoke, childhood respiratory illness, and a combination of genetics can also serve as factors leading to COPD diagnosis [1]. Anyone greater than 35 years of age with a smoking history or who has continuously experienced shortness of breath with activity, has a chronic cough and wheeze, has continuously higher than normal volume of sputum production, and/or has experienced consistent episodes of bronchitis during the cooler months, should be tested for COPD [7]. Several assessments can be used collaboratively to confirm the diagnosis of COPD. One tool for confirming a COPD diagnosis is spirometry, which measures the ratio of Forced Expiratory Volume (FEV 1) in one second divided by Forced Vital Capacity (FVC), amount of air expelled during FEV testing [6]. This calculated ratio is known as FEV1/FVC: A ratio below 0.70 confirms the presence of limited airflow [6]. Other tools to determine COPD severity include the COPD Assessment Tool (CAT) and the modified British Medical Research Council Questionnaire (mMRC), which can be used to assess COPD symptom severity in conjunction with spirometry [6].
The cost of care of COPD patients in the U.S. has reached $50 billion annually [1]. Nearly 23% of COPD affected patients that are age 65 and older are readmitted to the hospital for COPD exacerbation within one month of a previous admission. A COPD exacerbation is defined as noticeably increased shortness of breath or worsening cough, with sputum production, resulting in the need for oral steroids and antibiotics, increased rescue inhaler use, or hospitalization [8]. Temperature changes, allergy exposure, and flu or bacterial infection can trigger a COPD exacerbation [8]. According to Bourbeau, Saad, Joubert, and others, COPD admissions “contribute to a faster decline in FEV1 and worsening quality of life up to 14% of exacerbations take more than 35 days for resolution of symptoms and that more than 4% do not have complete recovery after 91 days” [9].
As a standard of care, the authors of the Global Initiative for Obstructive Lung Disease (GOLD) guidelines recommended pulmonary rehabilitation for people diagnosed with moderateto- severe COPD [10]. Authors of recent literature indicated that Pulmonary Rehabilitation (PR) programs positively affected patient self-efficacy and reduced COPD exacerbations that could lead to hospitalization [11]. PR is a multidisciplinary approach, used in conjunction with medication therapy, which involves exercise training, nutritional counseling, COPD education and management strategies, energy conservation techniques, breathing strategies, psychological counseling, and peer support for patients with various lung conditions, such as moderate-to-severe COPD [12]. Pulmonary rehabilitation programs that include an exercise educational component and that last a minimum of four weeks have shown to improve Quality Of Life (HRQoL) in COPD patients [13]. Most PR programs are 6-12 weeks and consist of 2 to 3 sessions per week [14]. In a PR study, Puhan et al. [15] disclose that 810 participants in eight different studies who completed a PR program demonstrated a 44% reduction in hospital readmissions and an improved distance of 62.4 meters during the 6-Minute Walk Distance (6 MWD) test.
A study conducted in 2013 posited evidence of improved 6 minute walk tests, improved exertion test scores (Borg’s score), as well as improvement in Chronic Respiratory Disease Questionnaire (CRQ) scores after just four weeks of rehabilitation [16]. Another study’s findings reveal that levels of fatigue improved by 60%, while dyspnea improved by 70% in over 1,600 participants who completed a minimum of four weeks of PR, as compared to people with COPD receiving standard care [17]. PR is strongly supported by evidence-based literature [18], “the effectiveness of PR is supported by highest-level evidence all patients will benefit, independently of the severity of their illness, even though the confirmed evidence is best for patients with moderate to severe COPD” [18]. The effects of pulmonary rehab include adding strength to muscle mass, reduction of exercise related shortness of breath, decreased hospital admissions and hospital length of stay, and improvement of self-efficacy and depression associated with COPD [18,19].
Despite the long-term benefits of pulmonary rehab, the recruitment process for rehabilitation has proven to be challenging [11], 170 people referred to PR services, 71 declined, with low enrollments the result of patient perception that PR exercise programs are too challenging to complete and being unaware that PR programs include an educational component [11]. Barriers to enrollment also included lack of family support, perceived inability to improve symptoms of advanced COPD, and patient perception that providers failed to present how PR could improve COPD symptoms and management [3]. Percentages of completion of pulmonary rehabilitation programs were as low as 3%-16% [3]. Other factors that lead to decline in participation in pulmonary rehabilitation included social isolation, poor support systems, increased COPD symptom burden, patient unawareness of PR program benefits, and lack of health provider promotion of pulmonary rehabilitation or follow through on the referral process [11].
The literature review was these electronic databases: PubMed, The Cochrane Library, Cumulative Index to Nursing and Allied Health Literature (CINAHL), Nursing and Allied Health, Health and Management, and Health and Wellness. Search terms included: pulmonary rehabilitation, COPD, adult, GOLD guidelines, outcomes, referral process, hospitalization, adherence, and the MeSH term pulmonary disease chronic obstructive. Articles included in the search were published from 2010 to 2018. Two applicable articles, both dated 2008, were mined from the reference sections of two articles included in the initial search. Articles used in the literature review included topics such as COPD exacerbations, PR referral process, reasons for declining in PR program uptake and completion, quality of life, COPD management, and COPD management guidelines. Inclusion criteria included participants with a COPD diagnosis, benefits of PR, COPD outcomes as a result of PR compared to standard care, barriers to PR, provider knowledge of PR, and peer reviewed articles. Articles not published in English, that were written prior to 2008, or that did not discuss COPD related outcomes as a result of PR were excluded from the review. Articles that focused on management of respiratory illness or PR referral due to a non-COPD diagnosis were also excluded from the review.
There were 249 articles accumulated for screening. After duplicate articles were removed from the review and inclusionary/exclusionary criteria applied, 237 records were screened, and 16 articles were included in the review (Figure 1). Following the methodology of Whittemore and Knafl, the integrative review was developed into sections, to include an introduction regarding COPD and the worldwide disease impact, a literature search, a data evaluation and analysis, a summary of the integrative review, and the conclusion of the review findings. Themes discussed in the review included hospital admission and health care cost reduction because of PR, barriers to pulmonary rehabilitation, and rehabilitation program enrollment and resultant effect on Health-Related Quality of Life (HRQoL).
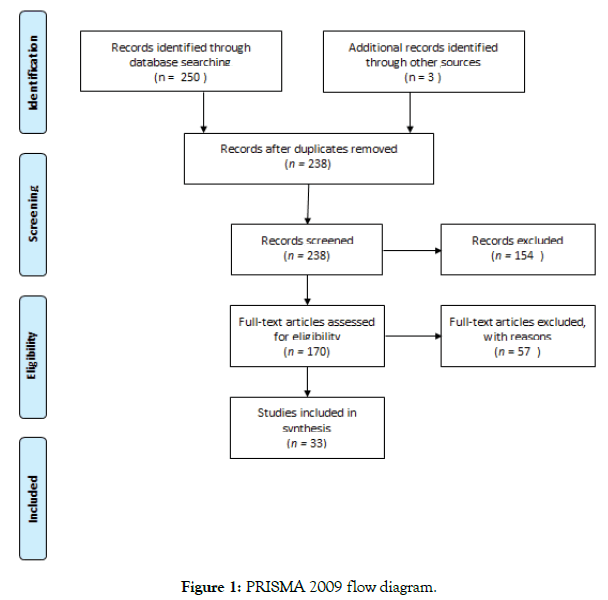
Figure 1: PRISMA 2009 flow diagram.
Data evaluation
Included in a summary of articles (Table 1) pertaining to PR and the link to reduced hospital admissions and overall health care costs determined by a 2018 study which shows pulmonary rehabilitation is linked to increased physical performance and improvement of dyspnea in COPD patients [18]. More research is needed to determine the appropriate PR regimen for patients with severe COPD and that collaboration between providers was imperative for better COPD outcomes [11]. Modifiable and non-modifiable factors such as gender, age, and smoking affect PR enrollment, but further investigation is needed to determine the best process for recruitment into PR programs [11].
| Study | Sample | Methods | Purpose | Conclusion |
|---|---|---|---|---|
| Cox et al. (2017) | People aged>18 years with diagnosis from 48 different studies |
Systematic review of qualitative and quantitative studies reporting data about referral, uptake |
To evaluate barriers and enablers to referral and participation to PR and map barriers to Theoretical Domains Framework (TDF) | Referrals to PR is the biggest barrier to enrollment to PR program, ranking 61% and falls under the Knowledge domain in the TDF |
| Gloeckl et al. (2018) | Selective literature search on German patients with severe COPD (N=750) |
Selective literature search in PubMed using search terms "pulmonary rehabilitation","COPD" | To present the importance of PR and its elements within the German health care system | PR improves physical performance, quality of life and dyspnea in patients with COPD |
| Man et al. (2015) |
Patients with recent COPD exacerbation who received PR from 9 RCTs (N=432) | 2015 Meta-analysis of the updated 2011 Cochrane Review of PR after COPD exacerbation |
To assess the effect PR has on rate of hospital readmissions for COPD exacerbation |
The precise format for supportive management after severe COPD exacerbation is unclear. A structured PR program requires more focus on appropriate collaborative care model going forward |
| Mathar et al. (2016) | COPD patients who were offered PR referral, but declined (N=170) |
Metasynthesis of seven studies compiled in 2014 regarding why patients decline PR referral |
To focus on correlations between gender, race, distance to PR, social support, smoking status, and decline of PR. |
PR enrollment could be enhanced if there is a streamlined referral process and if transportation is offered to PR location. Further investigation is needed to make PR more attractive to independent patients diagnosed with severe COPD |
| Revitt et al. (2013) | 160 participants with COPD who enrolled into outpatient PR program, 155 patients completed PR program and were counted in outcomes data | Cohort study consisting of enrolling 155 into 7-week PR program; hospital admissions were compared 12 months prior to PR completion to 12 months post PR completion | To determine if PR affects hospital readmissions for patients enrolled in PR program within 4 weeks of discharge from hospital for COPD exacerbation | PR completion after hospital discharge has a notable effect on hospital readmission for COPD exacerbation within at 12-month period of PR completion |
Table 1: Summary of articles- hospital admission and cost reduction.
There are many barriers to PR referral and enrollment, including lack of provider PR referrals, which contributes to low PR enrollments in the United States and worldwide [6]. A study conducted in 2015 emphasizes that COPD practice change across primary care clinics is necessary to increase referrals and patient knowledge of the benefits of PR [3]. Low awareness of PR is multifactorial and requires deeper investigation of COPD diagnosed patient populations in the primary care setting [20]. Two studies [21,22] explored patient uncertainty of benefits to overcome barriers to PR referral and patient adherence to PR in order to help health care providers better understand and overcome barriers to PR referrals.
Studies regarding the effect PR has on Health-Related Quality of Life (HRQoL) (Tables 2 and 3) encompassed physical activity, sedentary behavior, and dyspnea [23]. Dyspnea was the most associated disruption with HRQoL, which improves for patients who enroll into PR programs shortly after a COPD exacerbation [24,25].
| Study | Sample | Methods | Purpose | Conclusion |
|---|---|---|---|---|
| Cox et al. (2017) | People aged>18 years with COPD diagnosis from 48 different studies | Systematic review of qualitative and quantitative studies reporting data about PR uptake attendance/completion | To evaluate barriers and enablers to referral and participation to PR and map barriers to Theoretical Domains Framework (TDF) | Referrals to PR is the biggest barrier to enrolment to PR program, ranking 61% and falls under the Knowledge domain in the TDF |
| Foster et al. (2016) | Primary care physicians and NPs from 8 practices (N=22) |
Participatory action research design | strategies to influence clinician and patient behaviors to increase PR referrals | Primary care providers have limited knowledge of PR referral process. Practice change protocols and in-house, education will improve patient PR uptake |
| Greulich et al. (2015) | Patients with very severe COPD (N=544) | Retrospective analysis | To describe the effect of in-house PR program on patients with very severe COPD |
Patients with very severe COPD demonstrate improvement with PR |
| Hayton et al. (2012) | COPD patients referred to PR (N=711) | Retrospective analysis | To assess predictors of attendance and adherence to PR program | smoking status, family/friend support, COPD stage drive PR adherence |
| Johnston et al. (2012) | COPD patients with the average age of 76 years discharged for COPD exacerbation (N=15) | Observational Pilot Study | Explore implementation of key high evidence COPD guideline recommendations in admitted COPD patients | There is low awareness of PR referrals in patients and providers alike. A larger observational study is recommended to evaluate reasons for low awareness |
| Lewis et al. (2014) | COPD patients aged 42-90 (N=25) | Qualitative inductive approach within a phenonological framework using semi-structured interviews |
Determine experiences/expectations of COPD patients referred to PR program |
Recognizing uncertainty about PR is the first step to eliminate referral barriers |
| Spruitt et al. (2010) | Patients referred to PR who had COPD exacerbation focuses on two PR studies | Descriptive editorial | Discuss barriers leading to rejection of PR and methods to increase PR uptake | Access to PR is limited, providers and PR facilities must discuss and promote adherence |
Table 2: Summary of articles-barriers to pulmonary rehabilitation.
| Study | Sample | Methods | Purpose | Conclusions |
|---|---|---|---|---|
| Mesquita et al. (2017) | Patients with COPD (N=90 | Retrospective Observational Study | To evaluate patterns of change in physical activity and sedentary behavior after comprehensive PR program | One-third of COPD patients activity level improved after PR, whereas 1/3 of the patients did not improve. Focus is required on increasing daily light activity to improve activity level of the deconditioned patient |
| Monteagudo et al. (2013) | COPD patients >40 years of age from 21 primary care clinics (N=791) | Prospective Study | To identify factors associated with improved health-care related quality of life after 1 year follow up with primary care provider | About 1/3 of patients had increased health-related quality of life (HRQoL), 1/3 had decreased HRQoL. PR is linked to improved HRQoL. |
| Hayton et al. (2012) | COPD patients referred to PR (N=711) | Retrospective analysis | To assess predictors of attendance and adherence to PR program | smoking status, family/friend support, COPD stage drive PR adherence |
| Puhan et al. (2011) | COPD patients with COPD Stage II-IV (N=36) | Randomized Controlled Clinical Trial | Compare early v. late PR referral effects on HRQoL on patients with recent exacerbation | Early PR referral is associated with improved HRQoL |
| von Leupoldt et al. (2008) | von Leupoldt et al. (2008) | Quasi-Experimental Trial | To assess the effects of 3-week outpatient PR on HRQoL, exercise capacity, and dyspnea on COPD patients | PR reduces dyspnea, which in turn improves HRQoL |
| Yang et al. (2019) | Patients with COPD (N=1649) | Systematic Review and Meta-Analysis | A review of 17 RCTs to assess the effects of a minimum of 4 weeks PR on dyspnea, emotion, and fatigue | A minimum of 4 weeks of PR improves HRQoL including reduction of fatigue and dyspnea |
Table 3: Summary of articles- PR improves quality of life.
Data analysis
PR reduces hospital admissions and health care costs: COPD exacerbations that lead to hospitalizations have detrimental effects on patients’ respiratory symptoms, activity levels, levels of depression, and overall quality of life [26]. Over 700,000 hospital admissions in the United States are attributed to COPD exacerbation: Almost 20 percent of patients hospitalized for COPD are readmitted within a month contributing to over 17 million dollars in COPD related health care expenditures [27]. Patients who complete PR programs reduce risk of hospitalization and possible COPD related death up to four years post PR completion [28] Patients who enroll in a PR program shortly after a COPD exacerbation may be more motivated to implement lifestyle changes recommended by PR program, to reduce the risk of experiencing another stressful COPD exacerbation [28]. Statistics show that of patients readmitted to the hospital within 30 days for repeat COPD exacerbation, approximately 23% are Medicare recipients [29]. A Cochrane Review of six randomized controlled clinical trial posited that 57 out 100 people who had not completed a PR program experienced COPD related hospital readmissions while only 14 out of 100 patients who completed a PR program were hospitalized for COPD in a 34-week period after PR completion [28]. Nearly 20% of patients who experience a severe COPD exacerbation are readmitted to the hospital within 30 days, while approximately 30% are readmitted within 90 days [26]. A 2015 study demonstrated that 155 patients who completed four weeks of outpatient PR and 3 weeks of in-home PR had a 37.7% hospital readmission reduction 12-months post PR program completion [30]. A German study claimed that patients who completed a three week PR program immediately after a COPD exacerbation experienced a 22% reduction of hospital readmissions per year [18]. Authors from a 2015 study entitled Pulmonary Rehabilitation and Severe Exacerbations of COPD: Solution or White elephant determined that 432 patients hospitalized for COPD exacerbation that completed a PR program, there was a 22% hospital readmission reduction and a 29% mortality reduction [26]. PR programs lasting a minimum of three weeks in duration, preferably six weeks or more, lessened the intensity of exacerbations as well as increased the number of days to a subsequent exacerbation [27]. Patient exposure to a multidisciplinary PR program as soon as possible after COPD exacerbation was shown to definitively reduce hospital readmissions as patients as PR will help offset prolonged reduced mobility, therefore helping patients achieve baseline mobility more quickly [15,26].
Provider referrals PR rates as well as patient completion of PR regimen rates are very low as evidenced by a study that revealed only 90 out of 286 patients eligible for PR referral in a British hospital were referred to a PR program from November 2011 through late October 2012 [26]. On average, less than 5% of people who qualify for PR services receive a referral: Half of the patients referred to PR attend the initial PR session and only 30 % of referred patients graduate from a PR program [26].
Barriers to PR included lack of transportation, acute COPD exacerbation or other medical conditions such as heart disease that may potentially limit ability to perform PR program exercises, the perception that patients will not benefit from PR classes, history of smoking or use of long term oxygen, lack of support from family and friends, and provider lack of knowledge and support for PR [10]. Patients who live distances greater than 13 miles from a PR facility are more likely to decline a referral, as are patients who suffer from social isolation and are active smokers [10,21]. Other barriers to PR enrollment include patient perception of COPD prognosis as being too poor or not poor enough for rehabilitation, fear of repeat exacerbation after rigorous exercise, lack of continued encouragement from health care providers about the benefits of PR, lack of knowledge about the PR regimen, and the belief that a PR regimen will be too taxing for patients suffering from increased dyspnea on exertion [22].
Another barrier to PR referral is the lack of clarity in practice guidelines about which type of provider should refer patients and how to generate a referral to PR [3]. Provider discussions with patients about the benefits of PR, periodic provider focused PR educational in-services, improved and readily accessible COPD protocols that delineate how and when to refer patients to PR, and tools such as CDs or posters as reminders to refer patients to PR, are all necessary tactics to increase PR referral rates [3].
One physician, regarding the lack of awareness of PR referrals, stated: I think it is something that is not out there openly that we forget to be able to refer to, so I think if it was more publicized and that we had more awareness of these things being around that I think we would probably refer more people [20].
PR improves quality of life
Patients who do not attend PR often experience faster deterioration of lung function and experienced more frequent exacerbations, leading to decreased Health Related Quality of Life (HRQoL) [11]. Increased visits to a pulmonologist, smoking cessation attempts, and most importantly, participation in a PR program, are associated with a statistically significant increase in HRQoL in COPD patients [24]. In a study by Monteagudo et al. [22] out of the 28 participants who enrolled in PR, 16 participants scored higher on the quality of life scale known as the St. George’s Respiratory Questionnaire (SGRQ) [24] Of 210 participants in PR programs with duration of three weeks, a majority showed improvement in HRQoL [27]. A study by Leuopoldt et al. [23] involving an intensive 3-week 5 times per week pulmonary rehabilitation program determined that participants experienced less dyspnea, increased exercise tolerance, and overall improved HRQoL [25]. Instructors of pulmonary rehabilitation programs aimed to reduce time patients spend being sedentary, as increased dyspnea was associated most with poor quality of life [25]. A study by Mesquita et al. [21] discusses the measuring sedentary behavior after completion of a PR program: Out of 90 patients who completed PR 30% experienced a decline in physical activity [23]. Poor response or intolerance to PR is most likely due to deconditioning, consequently, PR programs and health care providers should promote daily and frequent light activity including but not limited to household chores such as folding laundry, which reduces sedentary behavior and improves overall quality of life as evidenced by reduced dyspnea on exertion and improved exercise tolerance [23]. According to Puhan et al. [28] enrollment into a PR program after COPD exacerbation results in decreased dyspnea at six-month follow up and quicker recovery time as compared to patients who are referred to PR 6-months after exacerbation [15]. Puhan et al. stated “early rehabilitation may lead to faster recovery of HRQoL after exacerbations compared to rehabilitation later on when patients are in a stable state” [15].
Limitations in the literature search include small sample sizes, contributing to difficulty in gathering generalizable evidence; therefore, larger population sizes are needed. Research is limited regarding efficacy of PR, therefore further studies are needed in the future. In the Johnston et al. study, although emphasis is placed on patients who have never received PR, there was not a discussion of this group of patients’ understanding of the benefits of PR. Educating patients who have not received PR about the benefits of PR while assessing barriers to completion of PR program is an important part of increasing PR awareness. Improved communication between providers and patients was an important aspect of a successful PR referral, therefore it improves communication between health care providers and patients if health care providers are aware of patient educational and cultural backgrounds.
Citation: Manzo LM, Jackson JC (2019) Pulmonary Rehabilitation Improves COPD Outcomes. Gen Med (Los Angeles) 7:325
Received: 29-Apr-2019 Published: 11-Jun-2019
Copyright: © 2019 Manzo LM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.